Nursing, Medical Schools Team Up on Simulation Collaborative
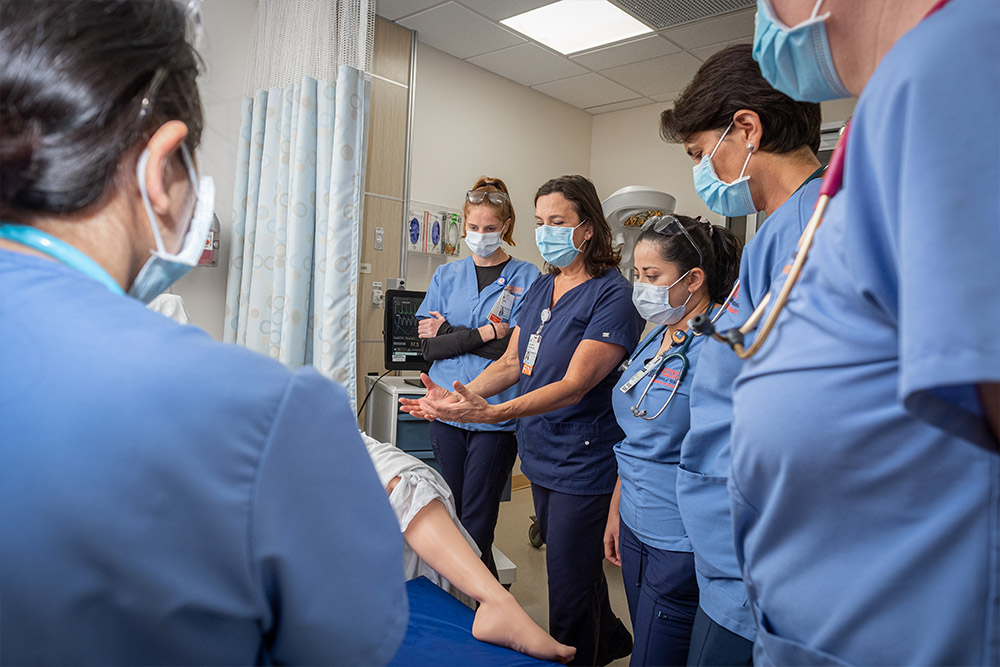
In early September, the University of Virginia School of Medicine and School of Nursing formalized a collaborative agreement between the two schools’ simulation centers to establish the University of Virginia Healthcare Simulation Collaborative. The goals of this agreement are to facilitate interprofessional and interdisciplinary collaboration, use space and resources more efficiently, and develop centralized personnel management to strategically match workloads. Combined, UVA will have more than 30,000 square feet of simulation space.
The ink had barely dried when the new shared-resources agreement was put into action. When one of the School of Nursing’s simulators broke down in September, the School of Medicine wheeled over a spare simulator. And, days later, when the School of Medicine needed several urinary catheter placement trainers, the School of Nursing offered theirs.
Going forward, such asset and space sharing will become common. Given that both Schools have specialized equipment to train students, but that some of it is only used a few times a year, sharing equipment simply makes sense.
30,000+
total number of simulation square feet available to nursing and medical students, with creation of the collaborative
The agreement also reduces costs. Simulation education is incredibly valuable but requires operational expertise and expensive equipment. By pooling our resources, we will decrease costs to obtain and maintain simulation tools and by sharing will require fewer devices in our fleet (and their accompanying pricey service contracts).
When students from both Schools have access to two simulation centers, simulation scheduling with also streamline. So when simulations are planned for the entire second-year School of Medicine class – that’s 52 simulations in a single week – we will be able to use both centers to double the number of simulation bays and ease the burden on faculty and staff — a move that ultimately makes for a better student experience.
All eligible simulation specialists in both centers are credentialed by the Society for Simulation in Health Care, an uncommonly achieved mark of excellence. It is our hope that in the future, UVA’s Healthcare Simulation Collaborative will be accredited as a single UVA entity. We will share more on this as it develops.
 READ MORE ABOUT THE SIM LAB'S 2021 CAPITAL EXPANSION
READ MORE ABOUT THE SIM LAB'S 2021 CAPITAL EXPANSION
The Best Part: Intangibles
Reducing costs is fantastic. Optimizing uptime on machines and fine-tuning schedules to maximize efficiencies is a beautiful thing. But the best parts of this agreement are the bonds that will naturally form through repeat collaborations.
Our Schools have incredible pools of talent. And our students are bright, energetic, and eager. Bringing medical and nursing faculty, staff, and students together to collaborate more regularly broadens our collective overall skillset and makes us more diverse. Building on that diversity, we hope to implement interprofessional education – a stated goal of each School – in new ways. Having faculty, staff, and students from nursing and medicine walk the same hallways and learn in the same spaces will spark conversations, friendships, and learning in ways for which we cannot plan.
Already, we see students from both Schools showing genuine interest in what the other group is learning when occupying the same rooms and hallways. To maximize these interactions, we plan to schedule our medical and nursing students to share the same spaces as much as possible.
There is power in combining expertise to drive and enrich simulation experiences and curricula, and develop new opportunities for interprofessional education and cross-team collaboration. These interactions will be fantastic for students (and their future patients) because, as we all know, healthcare is a team sport. Training together now means our medical and nursing students will be collaboration-ready in the future.
Ryan Ackard, assistant professor and the director of the Mary Morton Parsons Clinical Simulation Learning Center, will be the collaborative's new operations director.
Thank You, Faculty and Staff
None of this would be possible without the hard work, dedication, and commitment to medical education from team members in both Schools. Thank you to Vaia Abatzis, MD, Co-Director, Medical Simulation Center; Ryne Ackard, Director, Mary Morton Parsons Clinical Simulation Learning Center; Cathy Campbell, PhD, RN, Chair, Department of Acute and Specialty Care; Bethany Coyne, PhD, RN, Chair, Department of Family, Community & Mental Health Systems; Beth Epstein, PhD, RN, Associate Dean for Academic Programs; Allison Holt, Associate Dean for Finance & Administration; Keith Littlewood, MD, Assistant Dean, Clinical Skills Education; Stanley Lovett, Acting Director, School of Medicine Medical Simulation Center; John Teahan, Associate Dean for Administration; and our group of Simulation Operations Specialists who run the sim centers every day.
Through their efforts, we have combined two existing programs for the good of improving service to students, stewardship of resources, and professional education.
Meg Keeley, MD
Interim Senior Associate Dean for Education, School of Medicine
Harrison Distinguished Professor of Medical Education
Pam Cipriano, PhD, RN, FAAN
Dean, School of Nursing
Sadie Heath Cabaniss Professor of Nursing

