Moving the Needle on NPs' Autonomy
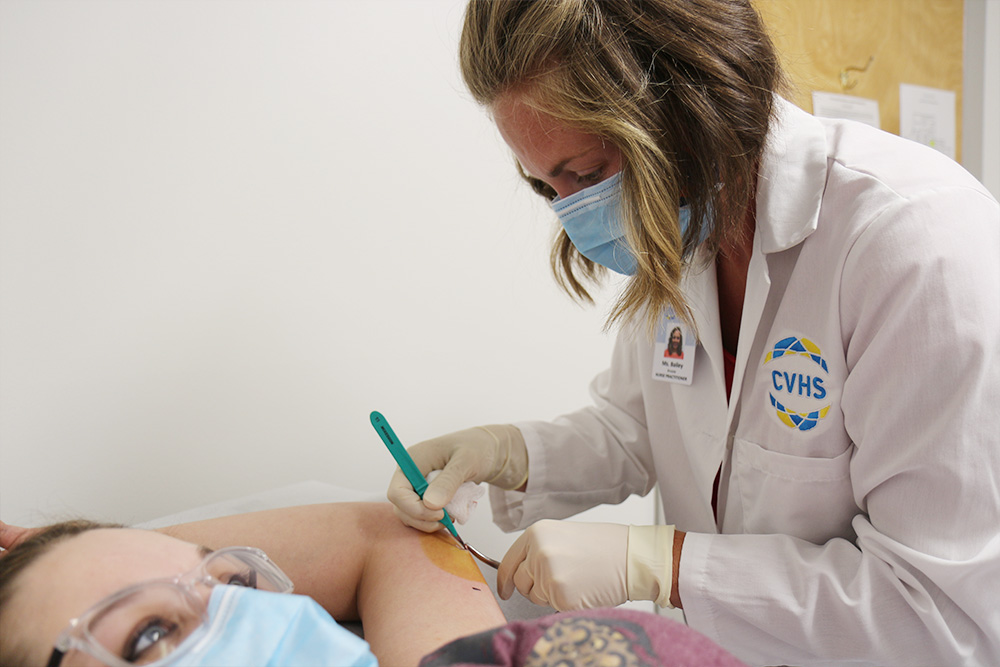
Brooke Bailey’s patients like to call her doctor—Dr. Brooke, Dr. Bailey, or just plain doctor—even though the family nurse practitioner repeatedly insists that she’s not one.
“They tell me, ‘I don’t care if you’re not a [medical] doctor,’” said Bailey, the first NP hired at Southern Albemarle Family Medicine in Esmont, Va., where she’s practiced since 2014, a clinic that provides primary care to thousands of patients from Buckingham to Madison, Richmond to Charlottesville. “You’re my doctor.”
29
the number of US states and territories that allow NPs full autonomy
Bailey, a University of Virginia School of Nursing graduate, is one of a small but growing number of NPs seeking to work independently—or “autonomously,” in industry jargon—untethered to a physician supervisor. And time is running out.
The COVID-19 pandemic opened a narrow legal window in Virginia for NPs like Bailey to apply for autonomy under relaxed standards, but that window is rapidly closing. She and others at the School of Nursing are trying to get the word out about the upcoming application deadline so NPs don’t miss this opportunity.
“Diagnosing, treatment, medication management, counseling, the list goes on,” Bailey said. “NPs are already doing it, so why not let us be autonomous? We are great providers, and we can be independent. We’ve got this.”

To address care gaps during the COVID-19 pandemic, an executive order from former Gov. Ralph Northam in early 2021 cut roughly in half the experience NPs needed to apply to practice autonomously. Instead of five years and 10,000 hours of practice, the order opened autonomy to NPs with two years and 5,000 hours of experience.
The idea was to augment NPs’ geographic mobility and provide more care to more people in the middle of a pandemic. And because NPs offer a wide spectrum of primary care—diagnosing and treating illness, ordering and interpreting tests, and prescribing medication—they are critical in ensuring access to healthcare both during and beyond pandemics, especially in rural areas where fewer physicians operate.
“NPs are already doing it, so why not let us be autonomous? We are great midlevel providers, and we can be independent; we’ve got this.”
Brooke Bailey, a family nurse practitioner at Esmont's Southern Albemarle Family Medicine who has applied for autonomy
Virginia is one of just 11 mostly southern states that require NPs to collaborate with a physician. After the window closes on July 1, Virginia will revert to the prior requirements governing their application for autonomy, rules that associate professor of nursing Kathryn Reid calls “antique.”
“There is an irrational fear that, with autonomy, NPs will go rogue, that we won’t collaborate anymore,” said Reid, a family nurse practitioner at the Greene Free Care Clinic and a three-term board member for the Virginia Association of Nurse Practitioners. “That’s nonsense. When we talk about what’s important to the health of Virginians, access to care is critical. And NPs are an important part of the solution.”
If more NPs garner autonomy, Reid explained, they will help bridge gaps in care, especially in Virginia’s 124 “health professional shortage areas,” home to nearly two million of the state’s 8.5 million residents.
More than half of states in the U.S. employ more relaxed NP licensure models than Virginia does, Reid said, who called the commonwealth “an outlier.” Those relaxed models are supported by the National Academy of Medicine and the National Council of State Boards of Nursing, and supported by the Federal Trade Commission, the American Enterprise Institute, and the American Association for Retired People, among other groups.
There’s another reason for promoting NP autonomy: It makes them want to stick around. Reid noted that many NPs who earn degrees from UVA often choose to practice in states with less restrictive practices, exacerbating Virginia’s “brain drain” of primary care providers.
“This piece of paper has no bearing on our clinical practice, except to satisfy the legal requirement,” said Reid, who also applied for autonomous practice earlier this spring.
The effort to ease Virginia’s nurse practitioner practice restrictions has been slogging on for more than a decade, championed by politicians like Delegate Dawn Adams (MSN `89), herself an NP, the Virginia Hospital and Healthcare Association, and the Virginia Council of Nurse Practitioners.
- In 2012, the state removed clinics’ requirement to have NPs supervised by on-site physicians, but they still had to have a collaboration agreement with a doctor.
- In 2018, a new law granted NPs with at least five years’ experience to apply to practice autonomously.
- And in 2021 came the executive order that opened autonomy to newer nurse practitioners. But it is a limited-time offer.
That narrow window afforded by the executive order is what pushed Bailey, who earned a master’s degree in 2014, to apply for practice autonomy earlier this spring. When she receives the letter confirming her autonomy later this summer, she said she’ll frame and hang it on her wall, next to her diplomas and nursing license.
“It’s paperwork, sure, but it’s also a statement saying, ‘We want this. Let’s do this,’” Bailey said. “It gives you an opportunity to fly.”
###


