Flashback Friday - RNs' Sept. 11 Response

“This is not the first time a little prop plane has hit the World Trade Center,” thought nurse Franklin Hickey (PhD `18) that bright sunny Tuesday, then director of patient care services at a 200-bed community hospital in New Jersey just 40 minutes outside Manhattan the morning of Sept. 11, 2001. It wouldn’t be long, however, before Hickey and his colleagues realized the gravity of the situation, and the immediate need to mobilize.
Eighteen years ago this week, 19 hijackers took control of four commercial airplanes and attacked both World Trade Center towers in New York City, and the Pentagon, in Washington, D.C. (A fourth plane crashed in rural Somerset County, PA). And while much has since been written about the disaster, emergency responders, and the trauma of witnesses near and far, it seems fitting this week to revisit 9/11 through a nursing lens.
One of many nurses there that day, Hickey’s 2018 dissertation—Doing Something: Oral and written narratives of nurses’ experience of the September 11, 2001 Disaster—analyzed themes across several nurses’ experiences, including his own, from different “Zones of Sadness,” a concept developed by psychoanalyst Charles Strozier to delineate individuals’ proximity to and visualization of chaos and horror.
Zone 1, said Crozier, is the closest area of trauma; those in Zone 2 witness disaster without experiencing death and destruction first-hand; individuals in Zone 3 could the burning Towers and were caught up in the evacuation process. Nurses like Hickey and his interviewees in New York and New Jersey experienced 9/11 in a very different way from those of us who watched the horror unfold on television.




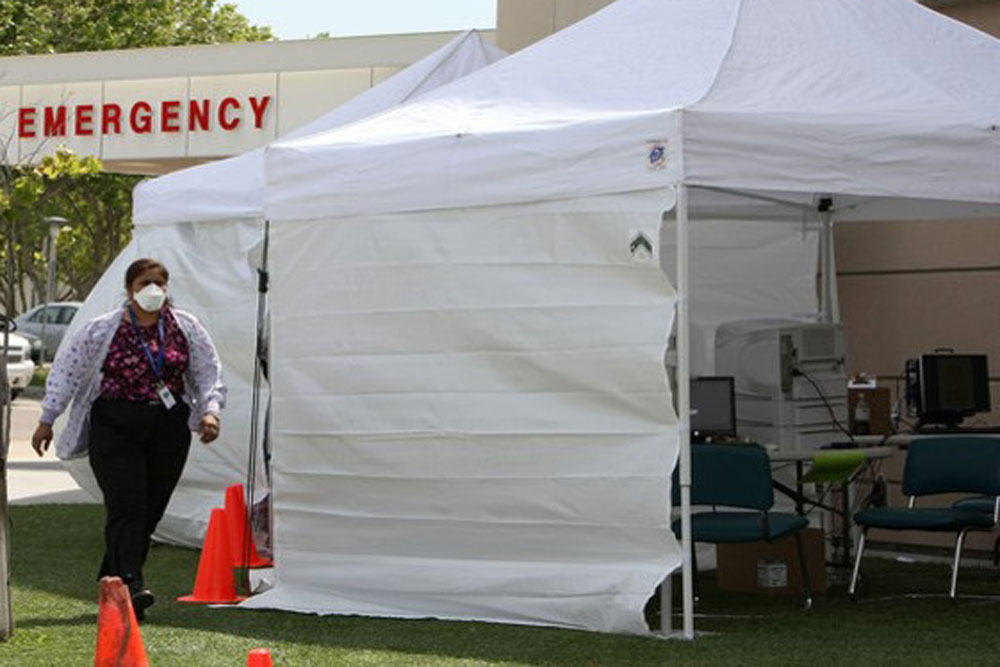


For Hickey, who became his hospital’s incident commander, a robust rapid response was met with the agony of waiting for patients to arrive. Communicating his hospital’s capacity state officials (150 beds, 15 in the ICU, 15 in the ER, and 10 surgical suites), Hickey and his team readied emergency supplies, erected a M.A.S.H.-style tent on the front lawn to expand capacity, and quickly transformed a classroom into a private room for overwhelmed staff. They readied the hospital driveway with stretchers, and cleared extra beds inside the OR, ER, and ICU.
By mid-morning, Hickey and his team fielded residents who sought safety and assurance, wished to donate blood, and offered donations. By 10:30 AM, he rounded to reassure patients and staff both, greeting off-duty nurses who’d begun arriving at the hospital, wishing to help. By 11 AM, Hickey heard that all roads throughout New York and New Jersey were closed.
The hospital was ready and willing to serve: where, he wondered, were the survivors?
By 12 noon, Hickey was advised to prepare for the “walking wounded.” By this time, Manhattan’s Bellevue and St. Vincents Hospital had already seen hundreds of patients, many with inhalation and eye injuries, chemical burns and lacerations. But at Hickey’s hospital, the quiet proved frustrating and eerie. It would be 8 PM before ambulances arrived with the first 15 patients who’d survived 9/11 with minor injuries, most so exhausted and in shock that they weren’t able to provide demographic information or even a complaint. Even without a psychological consult, Hickey’s nurses began to use depression screening tools, collaborating with physicians to determine the best treatment—responding the best they knew how.
By the end of the day, Hickey and his team assembled dormitories for staff who feared their commute, being alone, or were purely exhausted. Well after midnight, he fell asleep.
By 5 AM the following day, the rawness of tragedy came closer as Hickey and his team saw to the needs of ten children, ages 6 to 15, whose parents had worked in the towers and had not come home. In all, 30 percent of Hickey’s staff lost a relative or friend during the catastrophe. Heading home for the first time Sept. 13, Hickey clutched his 13-year-old son Frankie tight.
Nurses who responded to 9/11 faced situations that they’d never imagined possible. The stories they told in the aftermath offer a glimpse into what happened, and how in the years since they have processed and absorbed their part in helping.
“It was just incomprehensible, just absolutely,” recalled Bobbie Snyder, a New Jersey nurse who sought survivors with a cadaver sniffing dog in the rubble from Zone 1, whom Hickey interviewed. But “even though I was exhausted, none of us wanted to leave . . . That’s what our job is there for. That’s what we were there to do.”
Snyder also shared with Hickey a note she’d saved for years, which read:
“Dear Rescue Workers,
“Hello, my name is Raquel Maria Lopez, and I am sixteen years old. I attend St. Mary’s High School on 3rd street in downtown Jersey City. I don’t mean to take your time out of your rescue search, but I must tell you one thing; thank you. Thank you for going out there and trying to help everyone in need. Thank you for trying to find my aunt Nancy. Thank you for lending us all your strength and courage. It’s because of all you and our faith that we, the families, survivors, Americans, find what peace we do in such times. I want you to know that I will light a candle and say a prayer for you every night. You are true angels. You all hold a special place in my heart.
“I love you always,
“Raquel Maria Lopez”
###
This #FlashbackFriday brought to you by the Bjoring Center for Nursing Historical Inquiry. Special thanks to Franklin Hickey, PhD, for use of his dissertation, and to AAHN_Nursing president Arlene Keeling, professor emerita, for her guidance. #histnursing #histmedicine #nursing history

