'Sim Twins' Help Usher in New Pediatrics Master's Tracks
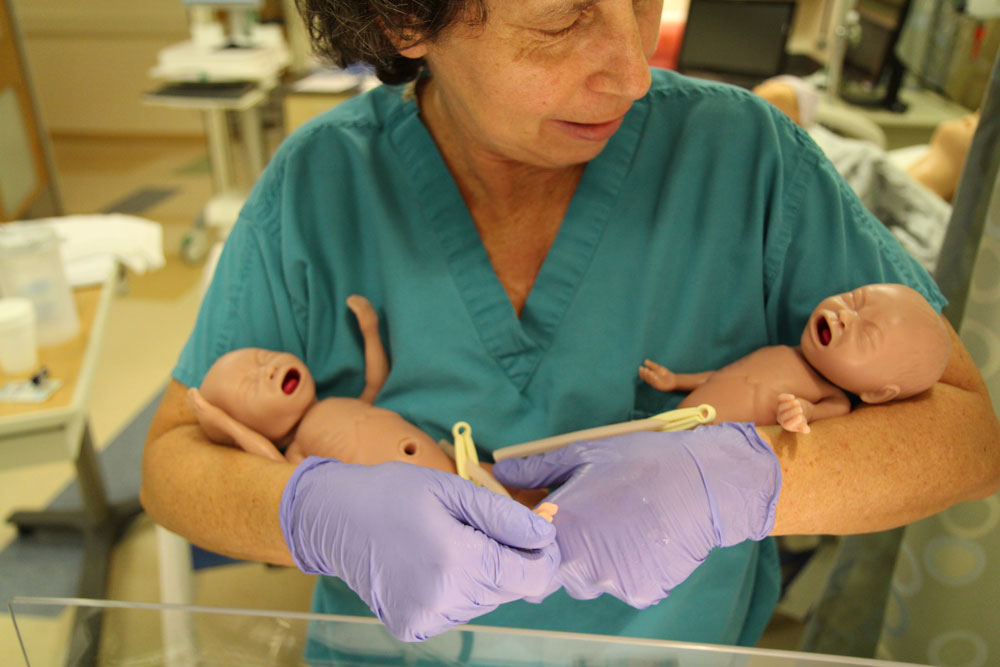
 The School's Clinical Simulation Learning Center’s (CSLC) phalanx of high fidelity humans has added two tiny new beings to the family: A pair of simulated premature infants, who breathe, cry, turn blue from low oxygen, run fevers, and can be ventilated, suctioned and receive IVs. The life-like “preemies” join the CSLC’s other simulators, which include several adults, and a series of newborn, toddler and five year-old sized devices.
The School's Clinical Simulation Learning Center’s (CSLC) phalanx of high fidelity humans has added two tiny new beings to the family: A pair of simulated premature infants, who breathe, cry, turn blue from low oxygen, run fevers, and can be ventilated, suctioned and receive IVs. The life-like “preemies” join the CSLC’s other simulators, which include several adults, and a series of newborn, toddler and five year-old sized devices.
The programmable infants – which mimic babies born between 23 and 27 weeks gestation, and cost $11,000 each -- come with a small, handheld computer, an umbilical cord, and a zippered backside where batteries nestle. They keep a charge for roughly four hours, say the CSLC’s staff, and, with their mannequin brethren, will become a regular part of the curriculum for students come summer, particularly those enrolled the School’s newest master’s tracks: the Neonatal Nurse Practitioner (NNP) and the Pediatric Nurse Practitioner-Acute Care (PNP-AC) programs.
“Access to this kind of technology is critical,” explains Barbara Reyna, an associate professor and NNP academic program coordinator, “and an integral part of the hands-on learning that’s needed to be a fully trained nurse practitioner in the neonatal and acute care pediatric setting.”
The new master’s tracks offer both full- (21 months) and part-time (33 months) study, and, given the need within both nursing specialties, many who struggle to hire qualified staff to tend vulnerable, sick children and infants, say it’s high time.
“We’ve heard for years from our colleagues that these remain areas of great need,” says UVA Nursing’s Christine Kennedy, associate dean. “That, coupled with RN retirements across the board and a growing demand for new nurse practitioners ready for the rigor of a NICU or PICU makes this a perfect time for our expansion.”
UVA Nursing’s new master’s tracks come at a time when such programs are few, a dearth that’s created corresponding decreases in neonatal nurses pursuing graduate degrees and available residencies to train them (Bellini, 2013). NNP and PNP-AC master’s and doctoral graduates account for less than two percent of nursing graduates nationally (AACN, 2015). Even as premature birth affects nearly ten percent of babies born in the US (March of Dimes, 2015) and hospitals strive to accommodate their care, the demand for nurses in these specialties remains acute.
With 45 percent of Virginia’s nurse practitioners set to retire in the next 15 years, a shortage of PNPs forecast over the next 13 years (Schell et al., 2015) and a 2013 study which found that 92 percent of American NICUs were understaffed due at least in part to a lack of qualified staff (Rogowski et al., 2013), the need across these specialties is critical.
Even with the 200 to 300 new NNPs entering practice across the US each year, demand far exceeds their supply, Reyna says. According American Association of Colleges of Nursing 2015 data, NNPs make up just 0.9 percent of the nation’s nearly 30,000 nursing master’s students and 1.3 percent of its graduates.
The same is true of PNP-AC students, who represent just 0.6 percent of the nursing master’s population, and one percent of its graduates (AACN 2015).
“With the mandatory decline in medical residents’ hours and a concurrent drop in the number of pediatric specialists, nurse practitioners are filling the gaps, and are in incredible demand,” explains assistant professor Bethany Coyne, a UVA pediatric nurse practitioner who, with PNP-AC Lisa Letzkus, directs the School’s PNP-AC track. “Given that they’ll be exposed to the wide variety of environments in which UVA Medical Center excels, these PNP graduates will emerge able to care for children across the continuum.”
Both NNP and PNP-AC students will complete more than 600 hours in clinical settings – at UVA Medical Center and a host of clinics and hospitals across the state and region – along with a courses specific to their specialty area. Working with gifted clinicians and academics, students will be exposed to a plethora of specialties and environments, including palliative and emergency medicine, ICUs, cardiology, hematology-oncology, and solid organ transplant units, among others.
“It’s vital that the NNP understand the contributions of maternal health and illness, and how that impacts fetal health,” explains Susan Almarode, a long-time NNP in UVA’s NICU and the clinical coordinator for the new NNP program, “but the practicing NNP must also appreciate the development progression and changing health status of the neonate into the infant and toddler as our practice covers birth to two years of age, intensive to primary care.”
It’s just the kind of experience that incoming student Casey Oot (NNP `19), of Austin, TX, calls a “huge motivator.”
“Becoming a nurse practitioner will give us a huge jump in terms of our autonomy and practice,” says Oot, who currently works in a Level III NICU. “You become part of a medical team, have a stronger influence in the practice, and make decisions in your specialty. As a bedside nurse, you’re part of research so far as its implementation, but to be a nurse practitioner means you get to investigate and be involved in the decision-making and opportunities you’re researching. I can’t wait to be a part.”
Jobs in these domains remain stable and well-paying. Neonatal nurse practitioners earn an average salary of $113,706 (salary.com, 2015) while pediatric nurse practitioners in acute care settings earn $93,041 to $101,204 (Advance Healthcare Network, 2015).
Applicants to the NNP must have at least a BSN and two years of NICU experience. PNP-AC applicants must have at least a BSN and a year of relevant nursing experience. Application deadline for both programs is in early January for entry the following fall.
